Oral & Maxillofacial Surgery of Westfield
6 Serious Health Problems Your Dentist Might Find
http://www.menshealth.com/health/health-problems-your-dentist-can-spot?cid=soc_MensHealthMag_TWITTER_Men’s%20Health__
Posted by
ronen908
on
Oct 30th, 2015
4:56 am
Posted in
Blog |
Comments Off on 6 Serious Health Problems Your Dentist Might Find
DENTAL IMPLANTS
DENTAL IMPLANTS
Your Teeth
The goal of dental implants is to replace a single tooth, several teeth, or all of the teeth in your mouth. You may have lost teeth from decay, gum disease, or an injury. Or, you may have a problem tooth that just needs to be removed and replaced.
There are 2 major parts to your teeth: the crown (which is the part you see), and the root (which is hidden below the gum line). Below the root are nerves that control feeling in your jaw, chin, tongue, gums, lips, and teeth. Above the upper jaw are your sinuses and nose. Sinuses are air-filled, bony pockets connected to your nose.
What are Implants?
Implants are small titanium that replace the root of your tooth. Your new tooth, bridge, or denture is placed on top of the implant. Dental implants look like, and have the strength of, natural teeth.
There are three basic parts to your final replacement tooth or denture. The implant is the post. And the “abutment” is attached to the implant and comes through the gums. When replacing a single tooth, the custom-made crown fits over this abutment.
Implants can replace a single tooth, several teeth in the same area, or all of the teeth in your jaw. The whole implant process can take anywhere from three months to a year, depending on your case.
Dr. Gold will place your implant, and your general dentist will fit your final replacement teeth. This is called “team treatment.”
Placing implants into your jawbone is surgery. Creating the new replacement tooth, bridge, denture, or full-arch prosthesis takes time. When replacing a single tooth or partial bridge, there is no such thing as having the implants placed and getting your final teeth the same day. It is possible to have your problem tooth removed, implant placed, and get a temporary tooth that day (although this is sometimes contraindicated.) Everyone’s situation is a little different. Dr. Gold will help you decide what’s best for you.
Before Your Surgery
Dr. Gold will examine your mouth and take certain x-rays to plan your treatment. When teeth are lost, the jawbone begins to shrink. Dr. Gold can use x-rays to see how solid your jawbone is and to look at its shape. Some patients may need a CT Scan (a special kind of x-ray) to show the position of their nerves or sinuses, and the shape and size of their jawbone.
Then, Dr. Gold will take a look at:
• The overall health of your teeth and gums
• How well you take care of your teeth
• How much jawbone you have
• Where the implant should be placed
• Your general health and health history
Dr. Gold needs to know:
• If you have any allergies
• What kinds of medications you take (including prescription and over-the-counter medications, herbal supplements, and vitamins)
• If you have a hip or knee replacement, heart murmur, or mitral valve prolapse
Dr. Gold may prescribe antibiotics for you to take before surgery to help prevent infections. One thing to know is that implants have a higher chance of failure in people who smoke. Some surgeons won’t place implants in smokers at all. The same is true for people who have diabetes but don’t control it very well and for those who drink alcohol heavily.
If you’re a good candidate, Dr. Gold will explain your treatment plan to you. This includes the number of implants you’ll need to support your new replacement crowns, bridge, or dentures. If your implants will hold bridges or dentures, you may have the choice of getting removable or fixed teeth. This is something to talk about with Dr. Gold and your general dentist who will be fitting your final teeth. If you don’t have enough bone or gum tissue to hold an implant, you might need to have some surgery to add more bone. This is called a “bone graft.”
Placing the Implant
Implants can be placed in 1 stage or 2 stages. Both approaches start the same way. Dr. Gold opens the gum tissue where the tooth is missing. A very precise drill hole is made into the jaw so that the implant can fit exactly. Dr. Gold then puts the implant into the hole.
1-stage implants
If you are having 1-stage implants, Dr. Gold may attach a healing collar that sticks through the gums. This collar gets the gums ready for the new tooth.
2-stage implants
If you are having a 2-stage implant, Dr. Gold will place a cover screw over the implant that does NOT stick through the gums. The gum tissue will be closed over the implant, usually with stitches.
Either way, you’ll have to wait anywhere between 3 to 6 months (usually 3-4 months) so your jaw bone and implant can fuse together. This allows your implant become strong and stable.
• In a 1-stage implant, a healing collar is already sticking through the gums. Once you get the okay, your general dentist can begin the process of making the final teeth.
• In a 2-stage implant, Dr. Gold will need to open up the gum area before placing the healing collar. You’ll wear this anywhere from 2 weeks to 1 month. Then, you’ll go to your general dentist to begin the process of making the final teeth.
After Your Surgery
After surgery, most people have very little pain.
• Dr. Gold will give you a prescription for antibiotics and pain medications to take as directed.
• It’s very important that you do not smoke for at least 2 to 3 weeks after your implants are placed. Smoking increases the chances of failure.
After you have your final replacement teeth fitted and made, cleaning those new teeth is very important. You need to keep those teeth even cleaner than you would your natural teeth. In fact, there are special mouth rinses that you could ask your dentist to prescribe for you.
How long can implants last?
Dr. Gold and your general dentist cannot guarantee a number of years. If you take good care of the implant or implants they could last you a long time.
Risks and Benefits
The benefits of implants
• A natural look
• A stronger bite
• An improved confidence in your smile
• Prevention of more bone loss
If you wear regular dentures, you know that they can come loose and be uncomfortable. Implants replace the root of the tooth, giving your replacement teeth a strong base so you can feel confident.
Implants also prevent future bone loss. When the root of your tooth is missing, the jawbone can start to shrink (which may change your facial appearance). Regular dentures cannot stop this bone loss.
Dental implants have a high success rate and are known to be very safe. But, like any surgery, there are some risks. There are some very rare and unusual risks that will not be covered here. Dr. Gold will discuss those risks as they pertain to your individual treatment.
Alternatives
Regular bridge
A regular bridge is made to replace one or two missing teeth. It’s cemented to the teeth on either side of the missing tooth. Your general dentist will need to grind down the neighboring teeth to make room for the caps. When taken care of, regular bridges can last many years.
Regular dentures
Regular dentures are another option. A complete denture sits on your gums. Everyday, dentures put pressure on your gums that can cause your jawbone to shrink. Because of this, dentures can come loose and lose their fit. Your general dentist can adjust your dentures regularly to improve the fit. But, over time, you could end up losing too much bone, preventing your dentist from making a well-fitting denture. If you are heading in this direction, implants may be your best choice.
As dental implants become more popular, you may hear news about them on TV or read reports in the media or on the Internet. Not all the information is good information. The best thing to do is talk it over with Dr. Gold or your general dentist to see if what you’ve learned makes sense for you.
Posted by
ronen908
on
Apr 17th, 2015
7:47 am
Posted in
Blog |
Comments Off on DENTAL IMPLANTS
Congratulations Dr. Gold!
Congratulations to Dr. Gold for being selected as a 2015 Top Dentist. It is the 7th year in a row that he has earned this honor. Dr. Gold thanks all of his colleagues for their confidence in him and for voting for him.
Posted by
ronen908
on
Feb 23rd, 2015
5:23 am
Posted in
Blog |
Comments Off on Congratulations Dr. Gold!
Wisdom Teeth
Wisdom teeth, also known as third molars, are the last teeth to erupt in your mouth. This generally occurs between the ages
of 17 and 25, a time of life that has been called the “Age of Wisdom.” Anthropologists note that the rough diet of early humans
resulted in the excessive wear of their teeth. Normal drifting of the teeth to compensate for this wear ensured that space
was available for most wisdom teeth to erupt by adolescence. The modern diet, which is much softer, and the popularity of
orthodontic tooth straightening procedures produce a fuller dental arch, which quite commonly doesn’t leave room for the
wisdom teeth to erupt, thereby setting the stage for problems when the final four molars enter the mouth.
What is an Impacted Tooth?
A tooth becomes impacted when there is a lack of space in the dental arch and its growth and eruption are prevented by
overlying gum, bone or another tooth.
How Serious is an Impacted Tooth?
Impacted teeth can be painful and lead to infection. They may also crowd or damage adjacent teeth or roots.
More serious problems may occur if the sac surrounding the impacted tooth becomes filled with fluid and enlarges to
form a cyst. As the cyst grows it may hollow out the jaw and permanently damage adjacent teeth, the surrounding bone and
nerves. Rarely, if a cyst is not treated, a tumor may develop from its walls and a more serious surgical procedure may be required to remove it. Despite the considerable concern regarding impacted third molars, a recent study sponsored by the American Association of Oral and Maxillofacial Surgeons and the Oral and Maxillofacial Surgery Foundation finds that third molars which have broken through the tissue and erupted into the mouth in a normal, upright position may be as prone to disease as those third molars that remain impacted. Complications such as infection, damage to adjacent teeth and the formation of cysts may arise from impacted teeth.
Must the Tooth Come Out if it Hasn’t Caused Any Problems Yet?
Not all problems related to third molars are painful or visible. Damage can occur without your being aware of it. As wisdom teeth grow, their roots become longer, the teeth become more difficult to remove and complications become more likely. In addition, impacted wisdom teeth are more likely to cause problems as patients age. No one can predict when third molar complications will occur, but when they do, the circumstances can be much more painful and the teeth more difficult to treat. It is estimated that about 85% of third molars will eventually need to be removed.
When Should I Have My Wisdom Teeth Removed?
It isn’t wise to wait until your wisdom teeth start to bother you. In general, earlier removal of wisdom teeth results in a less complicated healing process.The AAOMS/OMSF study strongly recommends that wisdom teeth be removed by the time the patient is a young adult in order to prevent future problems and to ensure optimal healing. The researchers found that older patients may be at greater risk for disease, including periodontitis, in the tissues surrounding the third molars and adjacent teeth. Periodontal infections, such as those observed in this study, may affect your general health.
What Happens During Surgery?
Before surgery, Dr. Gold will discuss with you what to expect. This is a good time to ask questions or express your concerns. It is especially important to let Dr. Gold know about any illness you have and medications you are taking. The relative ease with which a wisdom tooth may be removed depends on several conditions, including the position of the tooth and root development.
Impacted wisdom teeth may require a more involved surgical procedure. Wisdom teeth are easier to remove when the patient is younger, since their roots are not completely formed, the surrounding bone is softer, and there is less chance of damaging nearby nerves or other structures. Removal of wisdom teeth at a later age becomes more complicated as the roots have fully developed (may involve the nerve), and the jawbone is denser. Most wisdom tooth extractions are performed in the office under local anesthesia, nitrous oxide or intravenous sedation. Dr. Gold will discuss the anesthetic option that is right for you.
About Oral and Maxillofacial Surgery
Oral and Maxillofacial surgery is the specialty of dentistry that includes the diagnosis, surgical and adjunctive treatment of diseases, injuries and defects involving both the functional and aesthetic aspects of the hard and soft tissues of the oral and maxillofacial region.
An oral and maxillofacial surgeon is a graduate of an accredited dental school who has completed an additional four or more years of training in an accredited, hospital-based oral and maxillofacial surgery residency program.
Oral and Maxillofacial surgeons are an important link in the referral network for primary care providers. Through appropriate referrals, patients can be provided with expedient and cost-effective health care for conditions relating to the specialty of oral and maxillofacial surgery.
Posted by
ronen908
on
Dec 12th, 2014
7:11 am
Posted in
Blog, Wisdom Teeth |
Comments Off on Wisdom Teeth
Healthcare Provider CPR Re-Certification
On October 22, 2014, Dr. Gold and his staff hosted over 60 people for their CPR re-certification. The course was a huge success and everyone passed!
Posted by
ronen908
on
Oct 28th, 2014
6:08 am
Posted in
Blog |
Comments Off on Healthcare Provider CPR Re-Certification
Oral Cancer Fact Sheet
Prevalence
• An estimated 35,000 new cases of oral cancer will be
diagnosed each year.
• Oral cancer will claim 7,600 lives annually.
• On average, 60 percent of those with the disease will
survive more than five years.
• Oral cancer affects almost twice as many men as
women.
Risk Factors
• An estimated 25% of oral cancer patients have no
known risk factors.
• Alcohol and tobacco remain the greatest risk factors
(and using them in combination increases the risk 15
times over the use of one or the other);
• Infection with the sexually transmitted HPV16 virus
has been linked to a subset of oral cancers.
• Historically, oral cancer has been a disease of those
ages 40+, but its incidence in those under 40 has been
climbing.
• Prolonged sun or tanning bed exposure is a risk
factor for lip cancer.
• Smokeless tobacco is not a safe alternative to
cigarettes – users face a 400% greater chance of
oral cancer than non-users.
Possible Signs and Symptoms
• While you may have no symptoms at all, you should
see your oral and maxillofacial surgeon or dentist if
you experience any of the following:
– A sore on the lip or in the mouth that does not heal
– A lump or thickening on the lips or gums or in the
mouth
– A white or red patch on the gums, tongue, tonsils or
lining of the mouth
– Bleeding, pain or numbness in the lip or mouth
– Change in voice
– Loose teeth or dentures that no longer fit well
– Trouble chewing or swallowing or moving the tongue
or jaw
– Swelling of the jaw
– Sore throat or feeling that something is caught in the
throat
Early Detection
• Performing a self-examination regularly increases
the chance of identifying changes or new growths
early.
• If you have risk factors, also see your oral and
maxillofacial surgeon or dentist for an oral
examination at least annually.
• The earlier the cancer is detected, the easier the
treatment and the greater the chance of a cure.
Source: National Cancer Institute, National Institutes
of Health
Posted by
ronen908
on
Sep 8th, 2014
12:39 pm
Posted in
Blog |
Comments Off on Oral Cancer Fact Sheet
Dental Implant Surgery
More and more people are getting dental implants to replace missing teeth. They’re a long-term solution that is imbedded in your jawbone, just like your natural teeth. They even go your natural teeth one better, since they can’t develop cavities. Plus, unlike fixed bridges or removable dentures, dental implants will not affect neighboring healthy teeth or lead to bone loss in the jaw. If properly cared for, dental implants can last a lifetime.
Dental implant surgery is, of course, surgery, and is best done by a trained surgeon. Your oral and maxillofacial surgeon (OMS) has the specialized education and training in the complexities of the bone, skin, muscles and nerves involved, to ensure you get the best possible results.


 Implants are made of titanium metal that “fuses” with the jawbone through a process called “osseointegration.” There’s no short cut to get around that process, and it usually takes several months once the implant is put into your jawbone. Osseointegration, however, is why implants never slip or make embarrassing noises like dentures, and why bone loss is usually not a problem.
Implants are made of titanium metal that “fuses” with the jawbone through a process called “osseointegration.” There’s no short cut to get around that process, and it usually takes several months once the implant is put into your jawbone. Osseointegration, however, is why implants never slip or make embarrassing noises like dentures, and why bone loss is usually not a problem.
After more than 20 years of service, the vast majority of dental implants first placed by oral and facial surgeons in the United States continue to function at peak performance. More importantly, the recipients of those early dental implants are still satisfied they made the right choice.
Posted by
ronen908
on
Jul 24th, 2014
6:24 am
Posted in
Blog |
Comments Off on Dental Implant Surgery
Wisdom Teeth Management
Wisdom teeth, or third molars, are the last teeth to develop and appear in your mouth. They come in between the ages of 17 and 25, a time of life that has been called the “Age of Wisdom.” Wisdom teeth may not need to be extracted if they grow in completely and are functional, painless, cavity-free, disease-free and in a hygenic environment with healthy gum tissue. They do, however, require regular, professional cleaning, annual check-ups and periodic X-rays to monitor for any changes. When a tooth doesn’t fully grow in, it’s “impacted”–usually unable to break through the gums because there isn’t enough room. 90% of people have at least one impacted wisdom tooth. An impacted wisdom tooth can damage neighboring teeth or become infected. Because it’s in an area that’s hard to clean, it can also invite bacteria that lead to gum disease. Oral bacteria can also travel through your bloodstream and lead to infections and illnesses that affect your heart, kidneys and other organs. In some cases, a cyst or tumor can form around the base of the impacted tooth, which can lead to more serious problems as it hollows out the jaw and damages surrounding nerves, teeth and other parts of your mouth and face.
Generally, wisdom teeth should be surgically removed when there are:
- Infections and/or periodontal (gum) disease
- Cavities that can’t be restored
- Cysts, tumors or other pathologies
- Damage to neighboring teeth
The information provided here is not intended as a substitute for professional medical advice, diagnosis, or treatment. It is provided to help you communicate effectively when you seek the advice of your oral and maxillofacial surgeon.
Posted by
ronen908
on
Jun 16th, 2014
5:07 am
Posted in
Blog |
Comments Off on Wisdom Teeth Management
De-Stress for Better Oral Health
A furrowed brow, a tense look, a fresh acne breakout — you can often tell on sight when someone’s under pressure. If you could look into a stressed-out person’s mouth, you might learn even more of their story.
Stress and Your Mouth: What’s the Connection?
More and more researchers have been studying the link between stress and gum disease. When you’re anxious or depressed, your body produces more of the hormone cortisol. This compound harms your teeth and gums, contributing to the risk for periodontal (gum) disease.
There’s also evidence that stress and depression impair your immune system, making chronic infection throughout your body — including in your mouth — more likely. In addition, hard times lead to bad-for-your-teeth habits. These include smoking, drinking alcohol, and skipping your nightly brushing and flossing.
The following dental conditions also have been linked to stress, depression, or anxiety:
-
Burning mouth syndrome. This a painful condition that sufferers describe as a scalding feeling in the tongue, lips, and roof of the mouth.
-
Canker sores. Small, painful ulcers develop inside the mouth. Doctors aren’t sure what causes canker sores, but they are thought to appear more often when the individual is stressed or very tired.
-
Cold sores. These fluid-filled blisters are caused by the herpes virus. If you’re infected, you’ll often experience an outbreak in response to being upset.
-
Bruxism. People who grind their teeth (a problem called bruxism) tend to do it more when under stress. Grinding can wear and chip teeth and put pressure on jaw muscles and joints.
Ways to Relieve the Pressure
Don’t let your mouth take the brunt of your stress. Try positive stress-reducing techniques instead. Here are some strategies:
-
Change your outlook. Some things, like the weather, are out of your hands and for that reason are not worth getting worked up about. Try to see other life events as positive challenges rather than threats.
-
Keep your body healthy. Eat a nutritious, well-balanced diet and get enough sleep. And exercise on a regular basis. Not only will you get in shape and feel better overall, you’ll release anxiety and produce mood-boosting brain chemicals.
-
Practice relaxation techniques. These include meditation, stretching, and deep breathing and progressive relaxation of muscle groups.
“Bruxism.” Medline Plus, U.S. National Library of Medicine, National Institutes of Health, February 12, 2012. www.nlm.nih.gov/medlineplus/ency/article/001413.htm. Accessed 2013.
“Burning Mouth Syndrome.” National Institute of Dental and Craniofacial Research, National Institutes of Health, May 2011.www.nidcr.nih.gov/OralHealth/Topics/Burning/BurningMouthSyndrome.htm. Accessed 2013.
“Mouth Sores.” Mouth Healthy, American Dental Association. http://www.mouthhealthy.org/en/az-topics/m/mouth-sores. Accessed 2013.
“Relationship Between Stress, Depression and Periodontal Disease.” By A.M. M. Iacopino. Journal of the Canadian Dental Association. June 2009, vol. 75, no. 5, pp. 329-30. http://www.cda-adc.ca/jcda/vol-75/issue-5/329.pdf. Accessed 2013.
“Stress: How to Cope Better With Life’s Challenges.” American Academy of Family Physicians, November 2010.www.familydoctor.org/online/famdocen/home/common/mentalhealth/stress/167.printerview.html. Accessed 2013.
“Gum Disease Risk Factors.” American Academy of Periodontology. http://www.perio.org/consumer/risk-factors. Accessed 2013.
Posted by
ronen908
on
May 20th, 2014
5:03 am
Posted in
Blog |
Comments Off on De-Stress for Better Oral Health
One-Third of Americans Haven’t Visited Dentist in Past Year
Men, blacks, those with lower incomes, and Southerners less likely to see dentist
WASHINGTON, D.C. — About one in three U.S. adults say they did not visit the dentist at some point in the past 12 months. The 64.7% in 2013 who said they did visit the dentist at least once in the previous year is essentially unchanged from the rate found in 2008. Women are more likely than men to report visiting the dentist annually.
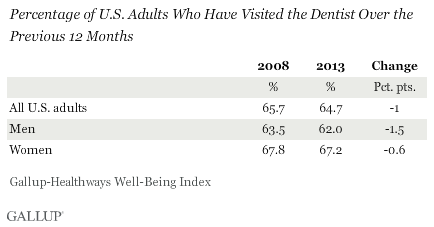
These findings are based on interviews with 178,072 American adults conducted during 2013 and with 354,645 adults conducted during 2008 as part of the Gallup-Healthways Well-Being Index. Respondents were asked whether they had visited the dentist in the previous 12 months. Results for all years between 2008 and 2013 are similar.
The American Dental Association recommends that adults develop a plan for dental visits with their dentist, but say even those at low risk of oral disease benefit from at least annual cleanings. Thus, one in three American adults do not meet this minimum level of dental care.
Blacks, Hispanics, and Young Adults Least Likely to Visit Dentist
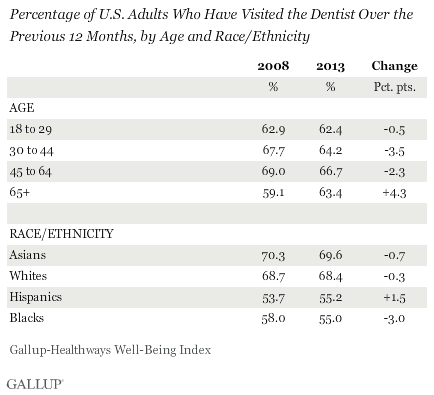
Among racial and ethnic groups, 55% of both blacks and Hispanics report visiting the dentist in the past year. Whites and Asians, in contrast, each are at about 70%, demonstrating that there is a notable racial and ethnic divide. Dental visit rates across most groups are similar to levels found in 2008, although there has been a small decline among blacks since that time.
In contrast, there are much smaller differences across age groups in reported dental behaviors. Young adults aged 18 to 29 are the least likely to have visited the dentist, but only marginally less so than those who are middle aged or older. An improved rate among seniors since 2008 is offset by a similarly sized decline among those 30 to 44.
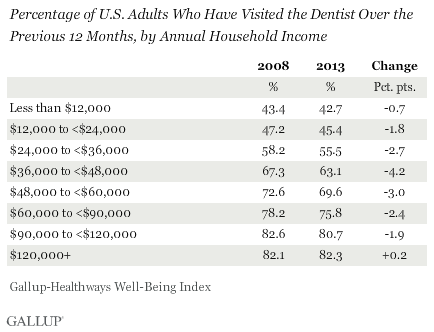
Dental Habits Improve With Income
The most pronounced differences in dental habits are those across income groups. Those who earn $120,000 or more annually in household income are about twice as likely as those who earn less than $12,000 to say they visited the dentist in the past 12 months, 82.3% vs. 42.7%, respectively. Dental visit rates have held steady since 2008 for top earners, while they have declined for all other groups, particularly for low- and middle-income households with incomes between $24,000 and $60,000 per year.
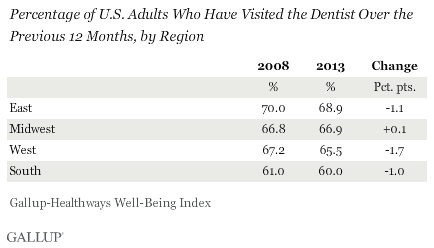
Annual Dental Visits Least Common in the South
Dental visit rates are essentially unchanged in all regions compared with 2008. As was the case in 2008, 2013 rates are lowest in the South (60.0%) and highest in the East (68.9%).
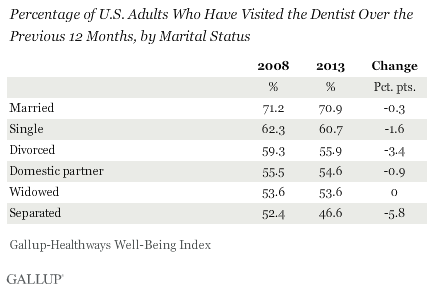
Married Adults Much More Likely Than Nonmarried to Visit Dentist
Marital status also influences dental decisions, with those who are married much more likely to report visiting the dentist annually than those who are not married. Those who are separated are the least likely to report visiting the dentist, and rates have dropped the most among this group — nearly six percentage points — since 2008.
Implications
Poor oral care can lead to many potential negative health outcomes. Recent medical research has indicated that when combined with other risk factors, poor oral health may be linked to both heart disease and stroke, possibly due to dislodged oral bacteria entering into the bloodstream. Maternal periodontal disease, too, has been linked to preterm births, and may increase risks for other diseases such as atherosclerosis, rheumatoid arthritis, and diabetes, among others.
The percentage of adults visiting a dentist in the past year varies widely across the major U.S. racial/ethnic boundaries, and may reflect several factors, including household income. Having health insurance coverage — which is related to income — also appears to be a meaningful factor in dental visits, although the Affordable Care Act may help minimize the disparities in professional dental care among income groups. According to the Congressional Budget Office, as many as 17 million adults could gain some form of dental coverage via the ACA over the next several years.
Regardless of income or insurance status, however, poor oral health is preventable. Health literacy, access, and motivation can all increase the likelihood of routine dental visits and help reduce the negative health outcomes associated with not visiting the dentist.
About the Gallup-Healthways Well-Being Index
The Gallup-Healthways Well-Being Index tracks well-being in the U.S. and provides best-in-class solutions for a healthier world. To learn more, please visit well-beingindex.com.
For results based on the total sample of national adults, the margin of sampling error is ±1 percentage point at the 95% confidence level.
The margin of sampling error for most demographic groups is less than ±1 percentage point, but is as high as ±2 points for groups with smaller populations, such Asians or those who are separated from their spouse.
Interviews are conducted with respondents on landline telephones and cellular phones, with interviews conducted in Spanish for respondents who are primarily Spanish-speaking. Each sample of national adults includes a minimum quota of 50% cellphone respondents and 50% landline respondents, with additional minimum quotas by time zone within region. Landline and cellular telephone numbers are selected using random-digit-dial methods. Landline respondents are chosen at random within each household on the basis of which member had the most recent birthday.
Posted by
ronen908
on
Apr 29th, 2014
11:28 am
Posted in
Blog |
Comments Off on One-Third of Americans Haven’t Visited Dentist in Past Year





